I 'm having a problem with Rigby, a 12-year-old male Lab mix diagnosed with pituitary-dependent Cushing's disease 3 years ago. We started him on trilostane (Vetoryl) at that time and the dog has done well, with complete resolution of clinical signs of polyuria and hair loss.
'm having a problem with Rigby, a 12-year-old male Lab mix diagnosed with pituitary-dependent Cushing's disease 3 years ago. We started him on trilostane (Vetoryl) at that time and the dog has done well, with complete resolution of clinical signs of polyuria and hair loss.
The owner called today and said that Rigby has been having urinary and defecation accidents in the house for 3 weeks. He has also been pacing, and possibly circling much of the night.
It sounds to me like the dog could be suffering from canine cognitive dysfunction. Can I use selegiline for canine cognitive dysfunction when the dog is already on treatment with trilostane? I was wondering, of course, because at one point in time selegilene was commonly used to treat Cushing's disease.
My plan is to first work the dog up to rule out an urinary tract infection, but do you have any other thoughts about the pacing and circling?
My Response:
First of all, your idea to do a workup for urinary tract infection (complete urinalysis with culture) is a good one and that should be the first step in your diagnostic testing. Urinary tract infections are common in dogs with Cushing's disease, even on treatment. If you haven't recently monitored the effects of trilostane treatment with an ACTH stimulation test, that should also be done at this time.
 If you believe that Rigby has canine cognitive dysfunction, you can certainly use the drug selegiline hydrochloride, also known as L-deprenyl (veterinary trade name, Anipryl) along with the trilostane that the dog's already getting.
If you believe that Rigby has canine cognitive dysfunction, you can certainly use the drug selegiline hydrochloride, also known as L-deprenyl (veterinary trade name, Anipryl) along with the trilostane that the dog's already getting.
As you know, Anipryl is approved by the FDA for use in dogs for treatment of pituitary-dependent hyperadrenocorticism, as well as canine cognitive dysfunction. This drug has fallen out of favor for treating dog's with Cushing's syndrome because it only partially controlled the disease in most dogs.
For cognitive dysfunction, some owners have reported marked improvement changes in their geriatric dog's behavior after starting Anipryl, while other dogs may not respond at all. Because of the drug's low incidence of side effects, however, it's certainly worth a try in dogs with suspected cognitive dysfunction.
I'd also recommend a good neurological exam. Remember that this dog has pituitary-dependent Cushing's disease. In most of these dogs, the cause have a pituitary ACTH-secreting tumor. With time, these pituitary tumors can grow and become large macrotumors, expanding and compressing the hypothalamus. That of course could be the cause of the dog's pacing as well. If that is suspected, a CT or MRI is recommended to confirm the presence of a large pituitary mass.
Źródło: endocrinevet.blogspot.com
She was initially started on NPH insulin at 0.4 U/kg BID (8 U BID). Over the course of 2 months, we increased the NPH dose to 0.7 U/kg BID (14 U BID) but the dog continued to be symptomatic. We did a blood glucose curve and obtained the following results:
- Fed at 7:30 AM
- Glucose at 8:30 AM: 132 mg/dl
- Glucose at 10:30 AM: 103 mg/dl
- Glucose at 12:30 PM: 160 mg/dl
- Glucose at 2:30 PM: 286 mg/dl
- Glucose at 4:00 PM: 381 mg/dl
Based on that curve was concerned that the duration was too short, so we switched to insulin detemir (Levemir). I know that detemir is more potent, so we started at 0.1 U/kg BID (2 units BID). The blood glucose curve 1 week later:
- Fed at 7:30 AM
- Glucose at 8:30 AM: 580 mg/dl
- Glucose at 10:30 AM: 343 mg/dl
- Glucose at 12:30 PM: 364 mg/dl
- Glucose at 2:30 PM: 361 mg/dl
- Glucose at 4:00 PM: 401 mg/dl
We then increased detemir to 3 units BID, and checked again 8 days later:
Fed at 7:30 AM
- Glucose at 8:30 AM: 422 mg/dl
- Glucose at 10:30 AM: 234 mg/dl
- Glucose at 12:30 PM: 253 mg/dl
- Glucose at 2:30 PM: 309 mg/dl
- Glucose at 4:00 PM: 381 mg/dl
We then increased to 0.2 U/kg BID (4 units BID), and checked again in 2 weeks.
- Fed at 7:30 AM
- Glucose at 8:30 AM: 422 mg/dl
- Glucose at 10:30 AM: 283 mg/dl
- Glucose at 2:30 PM: 356 mg/dl
- Glucose at 4:00 PM: 370 mg/dl
We just did a complete urinalysis and urine culture which was negative. Results of a recent CBC and serum chemistry panel were normal, except for the high blood glucose concentration. The dog is doing well clinically at home.
I'm not sure what to make of the persistent hyperglycemia on detemir. Possible Somogyi reaction? Or does the dog just needs more insulin?
When increasing the detemir insulin dosage, should I be going up a certain percentage or unit/half-unit at a time?
My Response:
This certainly doesn't look like an overdose of insulin or Somogyi overswing to me. Most likely, this dog just needs more insulin.
However, you should double check the following points with the owner as the next step:
- That they can accurately measure and then inject the insulin reliably.
- That they are feeding the dog only in morning and evening (no other treats during the day).
- That they are measuring the amount of food being feed, calculated by a veterinarian that it's the correct amount for the dog's ideal body weight.
 It doesn't appear clinically that she has any concurrent conditions that would cause insulin resistance, such as infection, inflammation, or Cushing's excess. Some dogs just require more insulin to adequately lower their blood glucose than do other dogs!
It doesn't appear clinically that she has any concurrent conditions that would cause insulin resistance, such as infection, inflammation, or Cushing's excess. Some dogs just require more insulin to adequately lower their blood glucose than do other dogs!In a large dogs, I increase my detemir dose by increments of 1 unit BID. In a small-breed dogs, I increase by less; by increment of 0.5 units BID.
I then wait 1 week or so and then repeat the serial glucose curve to make any additional needed dose adjustments.
Źródło: endocrinevet.blogspot.com

I came across something in one of my endocrinology books that indicates this may happen when starting thyroid supplementation, but this is the first time I've seen it in my 16 years of general practice. The skin scrape is negative, and there are no signs of any other skin pathology: there is no evidence of bacterial, yeast, or immune-mediated skin disease.
So do you think that this excessive shedding and flaking in this dog is related to initiation of the L-T4 therapy?
How frequently do you see this reaction or side effect?
What can I expect this dog's skin to do from here on? How long for this issue to resolve?
My Response:
Hypothyroid dogs occasionally develop severe shedding and flaking during the first 2 to 3 months of L-thyroxine treatment. During this time, the old telogen hairs are all being shed at the same time. With a bit of time on L-T4 replacement, the old shedded hairs are replaced with anagen hairs, and the skin cycle is restarted.
So I would expect the excessive shedding to resolve within the next 4 to 8 weeks on the L-T4 supplementation. However, you may want to treat the scaling symptomatically with a mild antiseborrheic shampoo and conditioner therapy such as Sebolux or Humilac. Adding some essential fatty acids (EFAs) to the dog's diet may also be of benefit.
If scaling persists or worsens beyond 8-weeks time, then skin biopsy for a keratinization disorder such as ichthyosis is recommended.
I can't give you an incidence for how often excessive flaking and shedding happens after initiation of L-thyroxine supplementation, but it certainly is not rare. I do see increased flaking more frequently in dogs with Cushing's disease during initial treatment with mitotane or trilostane than I do in dogs with hypothyroidism.
However, the reason I don't see this problem as often in hypothyroidism may simply be that, as a specialist, I only rarely get to treat and manage hypothyroid dogs. Although hypothyroidism can be a problem to accurately diagnose, it's an relatively easy disorder to treat.
Źródło: endocrinevet.blogspot.com
 Molly" is a 7-year-old Laborador Retriever weighing 31 kg, who was diagnosed over a year ago as being hypothyroid based on the finding of a low-normal serum T4 concentration (0.9 µg/dl; reference range, 0.9-3.9 µg/dl). Her clinical signs included non-pruitic alopecia of the pinnae and truncal dermatitis. Based upon her clinical signs and the low serum T4 value, she was started on L-thyroxine (Soloxine) a the dosage of 0.5 mg, BID.
Molly" is a 7-year-old Laborador Retriever weighing 31 kg, who was diagnosed over a year ago as being hypothyroid based on the finding of a low-normal serum T4 concentration (0.9 µg/dl; reference range, 0.9-3.9 µg/dl). Her clinical signs included non-pruitic alopecia of the pinnae and truncal dermatitis. Based upon her clinical signs and the low serum T4 value, she was started on L-thyroxine (Soloxine) a the dosage of 0.5 mg, BID.
Over the past year, a number of post-pill serum T4 concentrations have been done, but all of her serum T4 values have remained in the low-normal range (between 0.9-1.5 µg/dl). Her dose of Soloxine was increased to 0.6 mg but there still has not been improvement in clinical signs.
This week I repeated an entire thyroid panel while the dog is on the L-T4 and send the serum to the Michigan State University Endocrine Lab (animalhealth.msu.edu). Here are the results of that thyroid panel:
TT4: 59 nmol/L (15-67 nmol)
TT3: 1.5 nmol (1.0-2.5 nmol)
FT4: 20 pmol/L (8-26 pmol)
FT3: 5.2 pmol (4.5-12 pmol)
T4AA: 11% (0-20%)
T3AA: 5% (0-10%)
TSH: 0.01 mU/L (0-37 mU/L)
Thyroglobulin AA: 2% (0-35%)
My questions: Will being on L-thyroxine cause these numbers to all be normal? Is it advisable to stop the thyroid supplementation for a few weeks and run another serum thyroid panel, as clinically it doesn't seem to be doing much? Is she really hypothyroid at all?
Thank you so much for your help!
My Response:
Yes, the goal of thyroid hormone supplementation is to completely normalize the serum thyroid panel (i.e., to raise serum total and free T4 and T3 values and suppress serum TSH concentrations). So these results indicate that the L-T4 supplementation in this dog is being well absorbed and is feeding back on the pituitary gland to lower TSH secretion.
But you are correct: if the dog isn't hypothyroidism, the clinical signs aren't going to improve. I would recommend that you stop the L-T4 supplementation and redo the thyroid panel. Unfortunately, we need the dog off all L-T4 for at least 6 weeks prior to testing to allow the hypothalamic-pituitary-thyroid axis to recover. Once you stop the thyroid medication, this dog may be mildly hypothyroid (due to iatrogenic suppression of pituitary TSH secretion) even if his thyroid gland was normal prior to the thyroid supplementation.
When you do recheck Molly after stopping the thyroid mediation, remember to also run a CBC and serum chemistry panel. This will rule out any nonthyroidal diseases, but will also help in diagnosis of hypothyroidism, especially if mild anemia, or fasting hyperlipidemia/ hypercholesterolemia is present.
PS: I don’t know what the prior post-pill test results showed serum T4 values only in the low-normal range, but the serum T4 on this panel is perfect. Have the owners been consistently giving the L-T4 without food or at time of meals?
It’s been shown that absorption of L-T4 in dogs can be better when given on an empty stomach. So if the owners were not consistent in when they administer the thyroid medication, that could explain why the previous results were so different that the current results. And it may also explain why the dog hasn’t responded to the thyroid supplementation (if she really is hypothyroid, which still needs to be determined).
References:
1. Le Traon G, Burgaud S, Horspool LJ. Pharmacokinetics of total thyroxine in dogs after administration of an oral solution of levothyroxine sodium. J Vet Pharmacol Ther. 2008;31(2):95-101.
Źródło: endocrinevet.blogspot.com
 I read your recent post regarding Addison's disease and I'm writing to see if you could clear up (or add to the debate) a discussion that we are having at our hospital. I am a second-year medicine resident and our medical staff is having a debate about what is considered a normal vs. an abnormal cortisol response to ACTH stimulation and what exactly is "atypical" Addison's disease.
I read your recent post regarding Addison's disease and I'm writing to see if you could clear up (or add to the debate) a discussion that we are having at our hospital. I am a second-year medicine resident and our medical staff is having a debate about what is considered a normal vs. an abnormal cortisol response to ACTH stimulation and what exactly is "atypical" Addison's disease.
For example, what about dogs that have chronic gastrointestinal (GI) signs that have not yet been been diagnosed but a flat cortisol response to ACTH stimulation is found? If we perform an ACTH stimulation test on these dogs, many will have a basal cortisol level well within reference range limits (e.g., 2 to 4 µg/dl) but the post-ACTH stimulated cortisol concentration will not rise to levels 3-5 times higher than the basal cortisol concentration. Some of these dogs will have ACTH-stimulated cortisol concentrations that are below the post-ACTH reference range (e.g., in the range of only 3-6 µg/dl). Is this atypical Addison's disease?
What do you do in these cases? Look for other causes of the GI signs? And if no other cause found supplement with steroids? Should we just repeat the ACTH stimulation test down the line?
Thank you for your time!
My Response:
First of all, you must remember that the blog post on Addison's disease you are referring to was written primarily for dog owners, not veterinarians. I was trying to be clear, which is difficult when we are discussing a topic that could include typical, atypical, or secondary adrenal insufficiency.
Almost all dogs with primary hypoadrenocorticism (typical Addison's disease) and near complete destruction of the adrenal cortex will have subnormal basal and ACTH-stimulated serum cortisol concentrations (<1 μg/dl).
Dogs with secondary hypoadrenocorticism (pituitary ACTH deficiency) have low to low-normal basal cortisol values that may rise very slightly to ACTH stimulation, but the cortisol response is very blunted (post-ACTH values generally < 3 µg/dl). This has all been published (1-3), and I don't think anyone would strongly disagree with those guidelines.
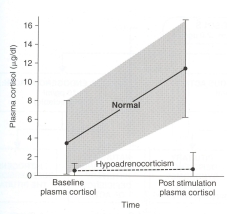
The problem with "atypical" Addison's disease is that, at least most of the time, the dogs have never been worked up properly to differentiate primary from secondary hypoadrenocorticism. Most would define "atypical" Addison's simply as glucocorticoid-deficient hypoadrenocorticism, but that is really being quite simplistic and does not help guide what replacement therapy may be needed or predict prognosis.
In other words, if that "atypical" dog has primary Addison's disease with normal electrolytes, it is very possible or even likely that mineralocorticoid replacement will be needed. On the other hand, it a dog has secondary hypoadrenocorticism, mineralocorticoid replacement will never be needed, but pituitary imaging (CT or MRI scan) might be indicated to exclude a pituitary mass.
The easiest way to differentiate primary from secondary hypoadrenocorticism, of course, would be to measure plasma ACTH concentration, but that must be done before any glucocorticoids have been administered (or after 1-2 weeks off all steroids).
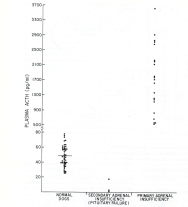
If the plasma ACTH value is low (generally < 20 pg/ml) in a dog with a severely blunted serum cortisol response to ACTH stimulation, that would be diagnostic for secondary hypoadrenocorticism (1-4). As you know, ACTH deficiency is rare and is most commonly associated with a pituitary tumor (3). By far the most common cause is iatrogenic secondary hypoadrenocorticism resulting from glucocorticoid administration. So it's extremely important in dogs with "atypical" Addison's disease to go back in the history and make sure that they haven't received any steroid in the last few weeks to even months.
If the plasma ACTH value is high (generally >250 pg/ml) with a severely blunted serum cortisol response to ACTH stimulation, that would be diagnostic for primary hypoadrenocorticism (1-4). If the serum electrolytes are normal, that could be called "atypical" Addison's disease. Some of these dogs will certainly go on to develop serum electrolyte changes, whereas others never seem to do so. I suspect that these latter dogs do not actually have adrenal destruction, but may have an ACTH receptor defect where circulating ACTH values are high but the adrenal gland doesn't bind the ACTH so it cannot act to stimulate cortisol secretion. Again, the best way to distinguish secondary from primary hypoadrenocorticism in these dogs is to measure plasma ACTH before any glucocorticoids are administered (or off all glucocorticoids for at least 1-2 weeks).
But let me get back to your original question about the dogs that have chronic GI signs and whose ACTH stimulation test results reveal a normal (or low) basal cortisol with a post-ACTH cortisol values that is blunted, rising to only 3-6 µg/dl. This is certainly not a "normal" response, abut it's very difficult for me to explain why these dogs would have any signs when these circulating cortisol values are within or slightly above the normal basal range. If this was a dog on mitotane or trilotane, for example, we would be very pleased with those serum cortisol results and would not be worried about hypoadrenocorticism (5-7).
In my experience, most of these dogs have a history of being treated with glucocorticoids, which could lead to secondary (iatrogenic) hypoadrenocorticism. Again, if you would measure a plasma ACTH concentration in these dogs, the values should be low-normal if they do indeed have secondary ACTH deficiency. If there is now history of glucocorticoid use, I would certainly repeat basal or ACTH-stimulated cortisol values in 2-4 weeks, but most of these dogs do not end up having primary adrenal disease.
Now that's not to say that they don't need steroid supplementation, but not for "atypical" adrenal disease.
References:
1. Peterson ME, Kintzer PP, Kass PH. Pretreatment clinical and laboratory findings in dogs with hypoadrenocorticism: 225 cases (1979-1993). J Am Vet Med Assoc 1996;208:85-91.
2. Kintzer PP, Peterson ME. Primary and secondary canine hypoadrenocorticism. Vet Clin North Am Small Anim Pract 1997;27:349-357.
3. Feldman EC, Nelson RW. Canine and Feline Endocrinology and Reproduction.Third Edition. Saunders, 2003.
4. Peterson ME, Orth DN, Halmi NS, et al. Plasma immunoreactive proopiomelanocortin peptides and cortisol in normal dogs and dogs with Addison's disease and Cushing's syndrome: basal concentrations. Endocrinology 1986; 119: 720-730.
5. Kintzer PP, Peterson ME. Mitotane (o,p'-DDD) treatment of 200 dogs with pituitary-dependent hyperadrenocorticism. J Vet Intern Med 1991;5:182-190.
6. Peterson ME, Kintzer PP. Medical treatment of pituitary-dependent hyperadrenocorticism. Mitotane. Vet Clin North Am Small Anim Pract 1997;27:255-272.
7. Ramsey IK. Trilostane in dogs. Vet Clin North Am Small Anim Pract 2010;40:269-283.
Źródło: endocrinevet.blogspot.com
 Prior to veterinary school, I worked as for a few years at a major medical center as a nurse in their endocrine clinic. In older human patients with hyperthyroidism, was not that uncommon for these folks to present with perfectly normal serum T4 values but have very high serum T3 concentrations.
Prior to veterinary school, I worked as for a few years at a major medical center as a nurse in their endocrine clinic. In older human patients with hyperthyroidism, was not that uncommon for these folks to present with perfectly normal serum T4 values but have very high serum T3 concentrations.
Do cats also develop a similar syndrome of T3 hyperthyroidism? That is, can some hyperthyroid cats maintain normal serum concentrations of T4 and free T4, but have clinical signs resulting from high circulating T3 values alone?
I've reviewed the literature, but I don't see that T3 thyrotoxicosis has ever been reported in cats. Is that because we just aren't checking serum T3 levels in hyperthyroid cats? Do you think that we are missing these cases?
My Response:
This syndrome is commonly referred to as triiodothyronine (T3) thyrotoxicosis or just T3 toxicosis. This disorder is found almost exclusively in the elderly and may be the cause of hyperthyroidism in up to 10% of older patients. T3 thyrotoxicosis is characterized by the finding of high serum T3 with normal or even low T4 levels, which can sometimes even lead to an erroneous diagnosis of hypothyroidism.
In the late 1970s and throughout most of the 1980s, we routinely measured serum T3 on all hyperthyroid cats. Although serum T3 concentrations were very high in many of these cats, we never documented a cat with isolated T3 thyrotoxicosis (1).
So over the last 35 years, I have certainly looked for this syndrome of T3 thyrotoxicosis. I have always expected to find some cats with normal T4 but high T3 levels, but to date the syndrome of T3 hyperthyroidism has yet to be documented in cats.
Today, we rarely use serum T3 concentrations as a diagnostic test for hyperthyroidism. Use of total T4 alone is diagnostic in over 90% of cats, whereas serum T3 values are high in only about two-thirds of cats (2).
That said, however, it still is possible that hyperthyroid cats could develop T3 hyperthyroidism. Certainly in circumstances where a low iodine diet is fed, you might see a situation where T3 is being secreted preferentially over T4 (3).
In states of iodine deficiency, it’s easier for the thyroid gland to make T3 compared to T4. The reason for that is simple — it takes one less iodide atom to make T3 than T4, since T3 only has 3 iodine atoms whereas T4 contains 4 iodine atoms. T4 has 1 more iodine atom than T3
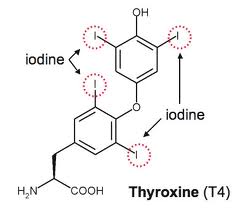
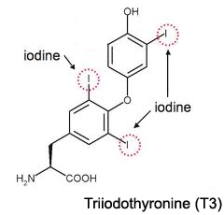
T4 has 1 more iodine atom than T3
Therefore, you have a cat in which hyperthyroidism is suspected, especially if a palpable goiter was present, but total and free T4 values are normal, I would certainly recommend that you run a serum T3 concentration to rule out T3 thyrotoxicosis.
References:
Peterson ME, Kintzer PP, Cavanagh PG, et al. Feline hyperthyroidism: pretreatment clinical and laboratory evaluation of 131 cases. J Am Vet Med Assoc 1983;183:103-110.
Peterson ME, Melian C, Nichols R. Measurement of serum concentrations of free thyroxine, total thyroxine, and total triiodothyronine in cats with hyperthyroidism and cats with nonthyroidal disease. J Am Vet Med Assoc 2001;218:529-536.
Laurberg P. Mechanisms governing the relative proportions of thyroxine and 3,5,3'-triiodothyronine in thyroid secretion. Metabolism: clinical and experimental 1984;33:379-392.
Źródło: endocrinevet.blogspot.com
 Today, May 25th 2011, we recognize the 4th Annual World Thyroid Day. Established in 2008, World Thyroid Day highlights five major goals to:
Today, May 25th 2011, we recognize the 4th Annual World Thyroid Day. Established in 2008, World Thyroid Day highlights five major goals to:
- Increase awareness of thyroid health,
- Promote understanding of advances made in treating thyroid diseases,
- Emphasize the prevalence of thyroid diseases,
- Focus on the urgent need for education and prevention programs, and
- Expand awareness of new treatment modalities.
In humans, dogs and cats, the thyroid, a large endocrine gland located in the neck, produces hormones that influence virtually every cell, tissue and organ in the body. The thyroid gland regulates the body's metabolism — the rate at which the body produces energy from nutrients and oxygen — and affects critical body functions, such as energy level and heart rate.
Diseases of the thyroid gland include hyperthyroidism, hypothyroidism, and thyroid cancer. These disorders are very common and affect tens of millions of people worldwide. As we all know from reading this blog, the same thyroid diseases are also common in dogs and cats.
For more information, see: www.worldthyroidday.com.
Źródło:animalendocrine.blogspot.com
Hyperthyroidism is one of the most common endocrine conditions affecting cats, especially older cats over the age of 10 years. Some veterinarians estimate that about 5 to 10% of middle- to old-aged cats will develop hyperthyroidism, and, due to factors that may include environmental exposures, that number is on the rise.
Thyroid hormones normally regulate many of the body’s metabolic processes. As circulating levels of thyroid hormones rise higher and higher in cats with hyperthyroidism, a progressive increase in their metabolic rate develops: this leads to a multitude of changes throughout the entire body, including loss of weight and muscle wasting. High thyroid hormone concentrations also interact with and stimulate the central nervous system, which commonly leads to increased activity or restlessness, as well as other behavior problems.
Clinical signs associated with hyperthyroidism can be quite dramatic and cats can become seriously ill with this condition. Untreated, hyperthyroidism in cats can lead to heart or kidney failure and can be fatal.
However, this disorder is a very treatable disease and most hyperthyroid cats will make a complete recovery. I’d discuss the various treatment options, together with pros and cons of each form of treatment, later in this current series of posts I’m doing on feline hyperthyroidism.
Do You Know the Clinical Signs of Hyperthyroidism to Watch for in Your Cat?
Here I’ve listed the top 10 most common signs that cats with hyperthyroidism can develop, from most common to least frequent.
Your cat doesn’t need to have all of these clinical signs or symptoms in order to have an overactive thyroid problem. But if your cat has one or more of these signs, especially if he or she is older than 10 years of age, you should definitely have your cat tested for hyperthyroidism.
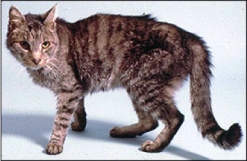 1. Weight loss
1. Weight loss
Weight loss despite a normal to increased appetite is the classic and most common sign of hyperthyroidism in cats. Hyperthyroidism is so common that it should always be considered as a possibility in any middle-aged to older cats that has lost weight, even in none of the other clinical features of the disease are present.
The weight loss associated is generally progressive and is usually first noticed by the owner as a loss of muscle mass around the cat’s back (spine).
With time, severe muscle wasting, emaciation, and death from starvation can occur if the cat’s hyperthyroidism is left untreated.
2. Increased appetite
The weight loss characteristic of cats with hyperthyroidism is typically associated with an increase in the cat’s appetite. This increase in appetite can be dramatic, with some cats doubling the amount of food eaten and frequently begging for food. Hyperthyroid cats eat more in an attempt to compensate for their higher-than-normal metabolic rate by increasing the number of calories ingested. Unfortunately, most cats cannot fully compensate and continue to loss weight even if they have a good to increased appetite.
 Although most hyperthyroid cats have an increased appetite, some cats with mild hyperthyroidism will maintain a normal appetite, with no obvious change in amount of food consumed.
Although most hyperthyroid cats have an increased appetite, some cats with mild hyperthyroidism will maintain a normal appetite, with no obvious change in amount of food consumed.
A few hyperthyroid cats will even develop a reduced appetite that is improved after treatment of their hyperthyroidism. Most of these cats with a poor appetite have a rare form of hyperthyroidism called “apathetic hyperthyroidism,” which is described in more detail below (see clinical sign Number 10).
3. Hyperactive, increased energy, or nervous behavior
Hyperactivity, exhibited particularly as nervousness or restlessness, is relatively common in cats with hyperthyroidism. In extreme hyperthyroidism, muscle tremor or twitching may be apparent, and affected cats are often described as having an anxious or frantic facial expression.
 In some cats, especially in the earlier stages of their hyperthyroidism, their owner can misconstrue such increased activity and energy as a positive sign of health. One must remember that cats normally become quite sedentary as they age so this change of behavior leading to increased energy and activity is almost always a manifestation of an underlying disease processes.
In some cats, especially in the earlier stages of their hyperthyroidism, their owner can misconstrue such increased activity and energy as a positive sign of health. One must remember that cats normally become quite sedentary as they age so this change of behavior leading to increased energy and activity is almost always a manifestation of an underlying disease processes.
Some of these behavior signs — especially restlessness or aggression — are often more noticeable to the examining veterinarian than to the cat owners themselves. Many hyperthyroid cats have an impaired tolerance for stress and do not wish to be held or restrained. Some will even develop a “panic attack” as a result of an impaired tolerance for examination or restraint during blood sampling. These cats may also develop panting, overt respiratory distress, weakness, and even collapse during these episodes.
To see a video of severe anxiety in a cat with severe untreated hyperthyroidism, see my previous blog post.
 4. Increased thirst and urination
4. Increased thirst and urination
About half of cats with hyperthyroidism will show signs of increased thirst (polydipsia) and urination (polyuria). Veterinarians often refer to polyuria and polydipsia simply as “PU/PD.”
There are a number of possible reasons for the increase in thirst and urination seen in hyperthyroid cats. The most common explanation for the PU/PD is mild, concurrent kidney disease. About a third of all cats older than 12 years of age will develop kidney disease, so the finding of concomitant kidney disease in a hyperthyroid cat should not be surprising.
Two other causes for polyuria and polydipsia in cats with hyperthyroidism include the following:
1. Increased kidney blood flow occurs secondary to hyperthyroidism, which can lead to what’s called “renal medullary washout.” This leads to the inability of the cat to concentration their urine normally.
2. Compulsive water drinking secondary to a behavior problem may also occur in some cats with hyperthyroidism.
In both groups of these cats, the increased thirst and urination return to normal after treatment of the cat’s hyperthyroidism.
5. Vomiting or regurgitation
Gastrointestinal signs including intermittent vomiting or regurgitation are fairly common in cats with hyperthyroidism. Vomiting may result from a direct action of thyroid hormones on an area of the brain called the chemoreceptor trigger zone. In other cats, the vomiting can result from gastric stasis (e.g., delay emptying of the stomach).
Vomiting appears to be more common in cats from multi-cat households and usually occurs shortly after feeding. Therefore, vomiting and regurgitation in most hyperthyroid cats may simply be related to rapid overeating. In other words, these cats eats too much food too fast, overfill their stomach, and then vomit.
One solution to this problem during the early stages of treatment is too feed the cat smaller amounts of food more frequently (every 3 to 4 hours, if possible).
6. Anxiety, night yowling, confusion, aimless pacing
The behavioral sign most obvious to owners is night yowling (a long loud mournful cry). This yowling most often occurs in the middle of the night for no apparent reason, and generally causes the owner to awaken. Aimless pacing and easily interrupted sleep patterns may also occur in some hyperthyroid cats.
All of these behavior signs appear to reflect a state of confusion, anxiety, or restless associated with the increased central nervous stimulation caused by the hyperthyroidism.
7. Diarrhea, soft stools, voluminous stools
Soft stools and diarrhea can occur in about a third of cats with hyperthyroidism. Other cats develop large voluminous stools with frequent defecation.
It is likely that accelerated gastrointestinal transit contributes to the increased frequency of defecation, soft stools and diarrhea. Some of these cats also develop malabsorption, in which they do not normally absorb the food from the intestinal tract.
8. Fast respiratory rate, panting, difficulty breathing
Respiratory abnormalities, including a rapid respiratory rate, panting, or difficulty in breathing at rest, are also common. Respiratory signs tend to occur most frequently during periods of stress. However, some affected cats will be noticeably intolerant of heat and seek out cooler places to sit, and some (especially advanced cases) may pant or breath more rapidly in warm or hot home environments.
In the absence of heart failure, weakness of the respiratory muscles due to chronic hyperthyroidism is the most probable reasons for these signs. However, central nervous or psychogenic effects also play a major role in development of these respiratory signs, especially in states of stress.

When severely stressed, some cats with hyperthyroidism will develop severe respiratory distress, rapid breathing, and panting; in addition, these cats may eventually become extreme weak or even collapse from exhaustion and shortness of breath. Hyperthyroid cats should therefore be handled carefully and in the veterinary office.
 9. Skin, hair coat, and nail changes
9. Skin, hair coat, and nail changes
Skin and hair coat changes often develop in hyperthyroid cats. The hair coat, especially in long-haired breeds, is often unkempt, dull, and may even be matted.
Some hyperthyroid cats can groom obsessively resulting in alopecia (baldness) or a miliary dermatitis (crusty rash, often with intense itching). This is sometimes associated with an underlying skin allergy, but the skin problem is magnified by the cat’s apparent obsessive and compulsive behavior associated with increased licking and grooming.
Excessive nail growth may also occur, especially in cats with chronic and advanced hyperthyroidism. These nails appear thickened and may be more fragile that normal.
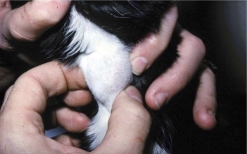
10. Apathetic hyperthyroidism
A small percentage (less than 5%) of hyperthyroid cats will show atypical signs where hyperexcitability or restlessness is replaced by depression, apathy, or weakness. Although weight loss is present in these cats, it is accompanied by poor appetite, instead of increased appetite. These disparate signs heighten the importance of clinicians having a high index of suspicion for such a common disease.

Many cats with apathetic hyperthyroidism will have concurrent severe non-thyroidal illness such as kidney failure, heart disease, or cancer. Therefore, it is wise to do a complete workup in these cats searching for secondary or concomitant disorders. Occasionally, however, no other medical problem can be identified and the cats respond completely to treatment of hyperthyroidism alone, with resolution of the depression and poor appetite.
In my next blog post, I’ll describe the 10 most common findings that your veterinarian may find when they perform a physical examination on a hyperthyroid cat.
Źródło: hanimalendocrine.blogspot.com







